Exploring health literacy, perceived needs, information preferences and acceptability of smartphone-based messaging interventions among individuals with obstructive sleep apnoea in Hong Kong: a mixed-method approach
Highlight box
Key findings
• There is low health literacy related to obstructive sleep apnea (OSA).
• A strong demand exists for authoritative health information.
• Messaging interventions were found to be acceptable for improving health habits and symptoms.
What is known and what is new?
• Technology’s role in disease management has gained prominence.
• This study highlights health literacy gaps related to OSA and emphasizes the importance of tailored health education to improve understanding and self-management.
What is the implication, and what should change now?
• Personalized interventions should be developed, guided by patients’ perceived needs and information preferences.
• A promising smartphone-based, innovative video messaging solution could be used to deliver health information, enhance treatment adherence, and improve overall outcomes for individuals with OSA.
Introduction
Background
Obstructive sleep apnoea (OSA) is a common chronic condition affecting about 12% of adults in Hong Kong and 24% in China mainland (1). OSA, characterised by intermittent hypoxia and sleep disruption, can lead to complications such as cardiovascular diseases (2) and metabolic disorders (3,4). Reviews and meta-analyses show that OSA is highly related to common health issues such as obesity (5), hypertension (6), diabetes mellitus (7), and hyperlipidaemia (4), as well as health-related behaviours such as smoking (8) and alcohol drinking (9). The American Thoracic Society recommends that overweight or obese people with OSA, regardless of their OSA severity, participate in comprehensive lifestyle interventions, including a reduced-calorie diet, regular exercise, and increased physical activity (10).
Digital technology is revolutionizing the management of OSA. Wearable devices like smartwatches track sleep patterns, heart rate, and oxygen levels (11). Mobile apps provide sleep insights and enable remote consultations (12). Connected continuous positive airway pressure (CPAP) machines offer real-time data, improve adherence, and adjust settings automatically (13). Data analytics, including machine learning, predict apnoea events and recommend personalised therapy (14). Virtual reality and artificial intelligence (AI) enhance diagnostics and treatment plans (15). These innovations improve diagnosis, adherence, and overall care for patients with OSA. In recent years, the role of technology in disease management has gained significant attention, with numerous studies exploring its application in conditions such as diabetes, asthma, chronic obstructive pulmonary disease (COPD), and cancer. For diabetes, a review demonstrated that mHealth apps tailored to diabetes management effectively improved glycemic control by significantly reducing hemoglobin A1c (HbA1c) levels in both type 1 and type 2 diabetes patients (16). Similarly, a systematic review of systematic reviews provided moderate-quality evidence that digital interventions increased smoking abstinence rates in asthma patients, contributing to better disease management (17). For COPD, three systematic reviews reported that digital self-management programs enhanced patients’ self-efficacy, improved dyspnea and quality of life, and reduced the risk of hospital admissions (18-20). For cancer patients, instant messaging interventions showed potential benefits in improving physical and psychosocial health outcomes (21).
Rationale and knowledge gap
However, mobile health technology for OSA remains underdeveloped, with limited research exploring its applications. Given the high mobile penetration rate in Hong Kong, leveraging mobile instant messaging for OSA self-management could be an innovative and cost-effective strategy. Evaluation of the clinical effectiveness of digital health technologies in improving health quality in real-world settings is urgently needed (22).
Objective
This study explored OSA individuals’ health literacy, perceived needs for improvement, information preferences, and acceptance of smartphone-based messaging interventions for support. It was hypothesised that a greater proportion of younger OSA individuals and those with a longer diagnosis duration would better understand the association between OSA and its related health conditions and habits compared to older individuals and those with a diagnosis of shorter duration, respectively. The findings can help develop a smartphone-based, patient-centred self-management support intervention to improve patient outcomes and relieve healthcare burden.
Methods
Study design and participants
This study included two parts. Part 1 was a cross-sectional, self-administered online survey using non-probability convenience sampling. It was conducted in both the inpatient ward and the outpatient clinic of a major university teaching hospital in Hong Kong from May to July 2020. To improve patient engagement, the questionnaire was designed with a larger font size (Font 14) to make it easier to read. For patients with poor eyesight or those who forgot their reading glasses, the research assistant provided support by reading the questions aloud and assisting them in completing the questionnaire. Part 2 was a focus group interview conducted in August 2020. This study was conducted in accordance with the Declaration of Helsinki and its subsequent amendments or comparable ethical standards. Ethics approval was obtained from the Institutional Review Board of the University of Hong Kong/Hospital Authority Hong Kong West Cluster (No. UW 20-068). The study was registered with the National Institutes of Health (identifier number: NCT04262986). All participants provided written informed consent.
Inclusion criteria included people who were (I) aged 18 or above, (II) diagnosed with OSA (with an apnoea-hypopnea index ≥5/hour) by polysomnography conducted in a sleep laboratory, (III) able to speak and read Chinese, and (IV) mentally fit to provide informed consent and complete self-administered questionnaires. We excluded participants who (I) were diagnosed with psychiatric illnesses, (II) had intellectual disabilities that presented difficulties in understanding and participating in the study, or (III) opted not to participate.
Data collection
Part 1, the self-administered questionnaire included health literacy, perceived needs, and views on smartphone-based messaging interventions to enhance self-management of OSA and its related treatment. which took around 10 minutes. In Part 2, nine participants from Part 1 were randomly selected and agreed to join a focus group interview to collect their perceived needs and views on smartphone-based messaging interventions. Table 1 shows the guiding interview questions.
Table 1
| Health literacy regarding OSA and related health conditions |
| What do you currently understand about the relationship between OSA and other health conditions? |
| Do you believe that lifestyle habits are linked to OSA? Why or why not? |
| How well do you understand the impact of untreated OSA on your overall health? |
| Perceived needs to improve OSA-related health, symptoms, and habits |
| What aspects of your health do you feel need improvement to better manage your OSA? |
| How motivated are you to make lifestyle changes? What challenges do you face in making these changes? |
| Information preferences |
| What type of information about OSA would you find most useful or relevant? |
| Where do you prefer to obtain information about OSA? Why? |
| Acceptability of smartphone-based messaging interventions |
| Would you find it helpful to receive health-related information through instant messaging apps like WhatsApp or WeChat? Why or why not? |
| What are the important components to include in messaging interventions? |
| How could we improve the video messages to make them more engaging and useful for individuals with OSA? |
OSA, obstructive sleep apnoea.
Measurement
Participants’ characteristics
Demographic and self-reported health information were collected including age (below 40, 40–49, 50–59, 60–69, 70 years old or above), sex (male or female), years since being diagnosed with OSA (less than 1, 1–3, 4–10, more than 10 years), severity of OSA (mild, moderate, severe, and unknown), current treatment related to OSA (CPAP, oral appliance, lifestyle modification alone, and others), and the presence of hypertension, diabetes, or hyperlipidaemia. Alcohol consumption and smoking habits asked by “In the past year, how often have you been drinking?” with the options “never”, “once a month or less”, “2–4 times per month”, “2–3 times per week”, and “4 times or more per week”; and “Do you have the habit of smoking?” with the options “yes”, “quit”, and “no”.
Health literacy on the association of OSA with its related health conditions and habits
Health literacy on the association of OSA with its related health conditions and habits (OSA-related health literacy) were assessed by seven questions: “Do you believe OSA is associated with being overweight, hypertension, diabetes, hyperlipidaemia, physical activity habit, smoking habit, or alcohol drinking habit?” with response options of “associated”, “not associated”, and “do not know”.
Perceived needs to improve OSA-related conditions, symptoms, and habits
Perceived needs to improve OSA-related conditions, symptoms, and habits were assessed by eleven questions in three categories. These included: “Do you think there is a need to improve your overall health condition, body weight, blood pressure, blood sugar level, blood lipid levels, sleep quality, snoring condition, fatigue, daytime sleepiness, physical activity habit, or dietary habit?” Response options were “greatly needed”, “needed”, “slightly needed”, “no needed” and “do not know”.
Information preferences
Preferences for receiving health information were assessed by five questions: “Would you be interested in receiving information on sleep quality improvement, OSA-related knowledge, weight control, health-related habits improvement, or emotional management?” Response options were “interested”, “not interested”, and “do not know”.
Acceptability of smartphone-based messaging interventions
Participants were asked about whether they installed instant messaging Apps (i.e., WhatsApp and WeChat) in their mobile phones, with response options of “yes” and “no”. The acceptability of smartphone-based messaging interventions was assessed across four areas: acceptability, perceived usefulness, preferred time and frequency of receiving messages. Acceptability was assessed by “Do you think it is acceptable to provide OSA and health-related information through messaging?” with response options of “acceptable”, “not acceptable”, and “do not know”. Perceived usefulness was assessed by “Do you think instant messaging could remind you to improve your health-related habits?” with response options of “yes”, “no”, and “do not know”. Preferences for the timing and frequency of instant messages were asked by “What time of the day do you think is most suitable for receiving health messages via WhatsApp or WeChat?” and “How many days per week would you like to receive health-related information?” The response options for the former were “morning”, “afternoon”, “evening”, and “night”, and for the latter “1–3 days”, “4–5 days”, and “6–7 days”.
Statistical analysis
The SPSS 25 software package (SPSS, Chicago, Illinois, USA) was used for data analysis. Descriptive statistics, including frequencies and percentages, were used to describe participants’ characteristics, beliefs regarding the association of OSA with related health conditions (such as overweight, hypertension, hyperlipidaemia, and diabetes), health-related habits (such as alcohol drinking and smoking habits), perceived needs for improving specific health conditions and habits, information preferences, acceptability and usability of instant messaging, and preferred timing and frequency of receiving health messages.
Linear regression was used to examine the association of OSA-related health literacy with age (<60 versus ≥60 years old) and year of diagnosis (<4 versus ≥4 years). Adjustments were made for variables including sex (male, female), education level (primary or below, secondary or above), year of diagnosis and age group. A “yes” response indicated that participants perceived a link between OSA and conditions like obesity, hypertension, diabetes, hyperlipidaemia, smoking and alcohol drinking habits. “No or not known” response indicated a lack of awareness or perception of these associations.
Qualitative data were coded and examined using NVivo 11 with thematic analysis, following the guidelines of Morse and Field (23). Two researchers (A.C.M.C. and H.W.H.T.) independently reviewed the interview materials, including transcripts and recordings, summarized the contents, and extracted meaningful statements. Field notes were also reviewed during the analysis. A research group, including the lead researcher (A.Y.K.L.) and the two additional researchers, discussed and resolved conflicting opinions regarding the themes identified. Mixed-method triangulation was adopted to interrelate and interpret quantitative and qualitative data. This triangulation strategy enhanced the authenticity and trustworthiness of the findings by converging information from different sources.
Results
Participants’ characteristics
Table 2 shows that of 108 participants who completed the questionnaire, 82.4% were men, and 40.7% were aged 60 years or above. Among the participants, 74% were married, and 60% had at least a secondary education. The majority (85.2%) were living with family or others, and 73.2% were employed. Additionally, 56.5% had been diagnosed for 4 years or more. The severity of OSA was reported as mild by 21.3%, moderate by 17.6%, and severe by 23.1%, but 38% did not know. Regarding treatment, 65.7% received CPAP, 4.6% used oral appliances, and 39.7% were prescribed lifestyle modification only. In terms of comorbidities, 60.2% had hypertension, 27.8% had diabetes, and 33.3% had hyperlipidaemia. Additionally, 9.3% were current smokers, 18.5% were ex-smokers, and 9.3% consumed alcohol two or more times per week. Nine OSA participants (78% male) participated in the focus group interview via Zoom.
Table 2
| Characteristics | n (%) |
|---|---|
| Sex | |
| Male | 89 (82.4) |
| Female | 19 (17.6) |
| Age | |
| Below 40 years old | 7 (6.5) |
| 40–49 years old | 16 (14.8) |
| 50–59 years old | 41 (38.0) |
| 60–69 years old | 36 (33.3) |
| 70 years old or above | 8 (7.4) |
| Marital status | |
| Married | 80 (74.1) |
| Never married | 19 (17.6) |
| Widowed/divorced | 9 (8.3) |
| Education level | |
| Primary or below | 19 (17.5) |
| Secondary | 46 (42.5) |
| Tertiary or above | 43 (40.0) |
| Living arrangement | |
| Alone | 16 (14.8) |
| Living with family/others | 92 (85.2) |
| Employment | |
| Employed, part-time | 6 (5.6) |
| Employed, full time | 73 (67.6) |
| Unemployed | 5 (4.6) |
| Retired | 20 (18.5) |
| Homemakers | 4 (3.7) |
| Years since being diagnosed with OSA | |
| Less than 1 year | 10 (9.3) |
| 1–3 years | 37 (34.2) |
| 4–10 years | 41 (38.0) |
| 10 years or above | 20 (18.5) |
| Severity of OSA | |
| Mild | 23 (21.3) |
| Moderate | 19 (17.6) |
| Severe | 25 (23.1) |
| I don’t know | 41 (38.0) |
| Current OSA treatment | |
| CPAP | 71 (65.7) |
| Oral appliance | 5 (4.6) |
| Lifestyle modification | 32 (29.7) |
| History of hypertension | |
| Yes | 65 (60.2) |
| No | 36 (33.3) |
| I don’t know | 7 (6.5) |
| History of diabetes | |
| Yes | 30 (27.8) |
| No | 73 (67.6) |
| I don’t know | 5 (4.6) |
| History of hyperlipidemia | |
| Yes | 36 (33.3) |
| No | 37 (34.3) |
| I don’t know | 35 (32.4) |
| Alcohol consumption in the past year | |
| 4 times per week or more | 6 (5.6) |
| 2–3 times per week | 4 (3.7) |
| 2–4 times per month | 13 (12.0) |
| Once per month or less | 28 (25.9) |
| Never | 57 (52.8) |
| Smoking habit | |
| Current smoker | 10 (9.3) |
| Ex-smoker | 20 (18.5) |
| Never smoker | 78 (72.2) |
Data are presented as n (%). CPAP, continuous positive airway pressure; OSA, obstructive sleep apnoea.
Health literacy on the association of OSA with its related health conditions, symptoms, and habits
Table 3 shows that 73.1% and 58.3% of participants believed that OSA is associated with obesity and hypertension, respectively. However, only 33.3% and 28.7% believed that OSA is related to hyperlipidaemia and diabetes. In terms of health-related habits, 38% of the participants believed there is an association between OSA and alcohol consumption, and 36.1% believed it is linked to smoking habits. No significant differences in the above by age and years of OSA diagnosis were found.
Table 3
| Health conditions and habits | All (n=108) | Age group† | Years of diagnosis‡ | |||||
|---|---|---|---|---|---|---|---|---|
| <60 years old (n=64) | ≥60 years old (n=44) | P value | <4 years (n=47) | ≥4 years (n=61) | P value | |||
| Obesity | 0.16 | 0.11 | ||||||
| Yes | 79 (73.1) | 50 (78.1) | 29 (65.9) | 38 (80.9) | 41 (67.2) | |||
| No or not known | 29 (26.9) | 14 (23.3) | 15 (34.1) | 9 (19.1) | 20 (32.8) | |||
| Hypertension | 0.90 | 0.16 | ||||||
| Yes | 63 (58.3) | 37 (57.8) | 26 (59.1) | 31 (66.0) | 32 (52.5) | |||
| No or not known | 45 (41.7) | 27 (42.2) | 18 (40.9) | 16 (34.0) | 29 (47.5) | |||
| Hyperlipidemia | 0.66 | 0.41 | ||||||
| Yes | 39 (36.1) | 22 (34.4) | 17 (38.6) | 19 (40.6) | 20 (32.8) | |||
| No or not known | 69 (63.9) | 42 (65.6) | 27 (61.4) | 28 (59.6) | 41 (67.2) | |||
| Diabetes | 0.26 | 0.28 | ||||||
| Yes | 31 (28.7) | 21 (32.8) | 10 (22.7) | 16 (34.0) | 15 (24.6) | |||
| No or not known | 77 (71.3) | 43 (67.2) | 34 (77.3) | 31 (66.0) | 46 (75.4) | |||
| Smoking | 0.46 | 0.57 | ||||||
| Yes | 47 (43.5) | 26 (40.6) | 21 (47.7) | 19 (40.6) | 28 (45.9) | |||
| No or not known | 61 (56.5) | 38 (59.4) | 23 (52.3) | 28 (59.6) | 33 (54.1) | |||
| Alcohol drinking | 0.49 | 0.21 | ||||||
| Yes | 41 (38.0) | 26 (40.6) | 15 (34.1) | 21 (44.7) | 20 (32.8) | |||
| No or not known | 67 (62.0) | 38 (59.4) | 29 (65.9) | 26 (55.3) | 41 (67.2) | |||
Data are presented as n (%). †, between-group differences of variables adjusted for sex (male, female), education level (primary or below, secondary or above) year of diagnosis (<4 and ≥4 years); ‡, between-group differences of variables adjusted for sex, education level (primary or below, secondary or above), age group (<60 and ≥60 years old). “Yes” indicated that respondents perceived an association between OSA and specific health conditions (obesity, hypertension, diabetes, and hyperlipidemia), as well as smoking and alcohol consumption habits. “No or not known” indicated that respondents were either unaware of or did not perceive any association between OSA and specific health conditions (obesity, hypertension, diabetes, and hyperlipidemia), as well as smoking and alcohol consumption habits. OSA, obstructive sleep apnea.
During the focus group interview, some participants reported that they did not fully understand what OSA and its related diseases are.
“Although I was diagnosed with sleep apnea some time ago, I didn’t fully understand what this condition is. I only knew that the doctor asked me to use the machine, so I followed their advice and used it.” (male, aged 56 years, OSA diagnosed >10 years).
“I didn’t know that OSA could actually lead to heart disease until you explained it to me just now.” (female, aged 51 years, OSA diagnosed >10 years).
Perceived needs to improve OSA-related health conditions, symptoms, and habits
Figure 1 shows that 76.8% of participants reported a need to improve their overall health conditions, 71.3% to improve their body weight, 52.7% to improve their blood pressure, 44.5% to improve their blood lipid levels, and 37% to improve their blood glucose levels. Regarding OSA-related symptoms, 61.1% reported a need to improve their sleep quality, and 56.4% to address their snoring condition, 52.5% to alleviate fatigue, and 45.4% to reduce daytime sleepiness. Regarding health-related habits, 63.7% reported a need to increase their physical activity, and 58.3% to improve their dietary habits.

During the focus group interview, participants reported disease- and treatment- related information was particularly important for those newly diagnosed with OSA and new CPAP users. They preferred reliable information from authoritative institutions.
“I believe it’s better to obtain information from hospitals and universities, rather than relying solely on YouTube or public media. Some information from media platforms can be misleading, and it is difficult for us to factcheck. Besides those disease- and treatment-related information was important for those newly diagnosed and new CPAP users.” (Male, aged 54 years, OSA diagnosed >10 years).
“I always wake up in the middle of the night, and I really want to improve—not just my apnea issues but also the problem of waking up during the night.” (female, aged 50 years, OSA diagnosed <10 years).
Information preferences
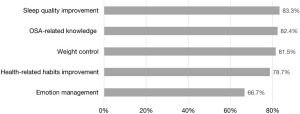
Figure 2 shows that the preferred information included information related to sleep quality improvement (83.3%), OSA-related knowledge (82.4%), weight control (81.5%), improvement in health-related habits such as physical activity and dietary (78.1%), and emotional management (66.7%).
During the focus group interview, participants reported that disease- and treatment-related information was particularly important for those newly diagnosed with OSA and new CPAP users. Furthermore, diet-related information was the most welcomed and highly valued.
“I will pay more attention to it when it is about CPAP machine or mask instructions. I never knew a chin strap could fix the air leakage problem.” (male, aged 58 years, OSA diagnosed >10 years).
“Since we love eating, it is good to introduce some healthy cooking methods for different types of food.” (female, aged 51 years, OSA diagnosed >10 years).
Acceptability of smartphone-based messaging interventions
Ninety-eight percent of the participants owned a smartphones, 95.4% used WhatsApp, and 51.9% used WeChat. Figure 3A shows 82.4% believed that sharing health-related information via instant messaging is acceptable. Most (72.2%) believed e-health information can remind them to improve their health-related habits, and 71.3% were willing to share the received health messages with their family or friends. Figure 3B shows that the preferred time for receiving health messages were in the morning (33.3%) and at night (35.2%). Figure 3C shows that 68.5% preferred receiving health messages one to three days per week.

During the focus group interview, participants also suggested using short easy-to-understand video messages and a scoring system to encourage watching the video messages, and a real case-sharing video can help motivate participants to exercise more.
“It would be nice to have 2- to 3-min video messages to deliver health information, because of the poor eyesight. The content is easy to understand. Besides, it was good to have a scoring system for us to follow. Let’s say: add 5 marks for watching a video and participants may redeem presents according to their scores.” (female, aged 51 years, OSA diagnosed >10 years).
“I am not sure about the effectiveness of the exercise program you have provided daily. So, it would be great if there were real case sharing and the participants be told that the goals could be achieved.” (male, aged 58 years, OSA diagnosed >10 years).
Discussion
Key findings
Our study is the first to report OSA-related health literacy, perceived needs, information preferences, and the acceptability of smartphone-based messaging interventions. The findings revealed low OSA-related health literacy among individuals with OSA in Hong Kong, with no significant differences observed across age groups or years since OSA diagnosis. Participants also demonstrated a strong desire to improve their health, a high demand for OSA-related information, and good acceptability of OSA messaging interventions.
Comparison with similar research
First, our finding shows more than half of the participants were aware of the association between OSA and obesity (73.1%) and hypertension (58.3%), but only about one-third were aware of its association with alcohol consumption (38%), smoking (36.1%), hyperlipidemia (36.1%), and diabetes (28.7%). A scoping review of reviews found that participants with limited health literacy often encounter difficulties in specific self-management domains, such as lifestyle adjustments and symptom monitoring (19,24). Developing critical health literacy abilities is more effective for enhancing self-management behaviours than relying solely on social support, especially for people with multiple chronic diseases (20,25). In the current study, we found no significant difference in OSA-related health literacy between age groups (<40 vs. ≥40 years old). This indicates that these findings contrast with Chiu et al., who reported age as an influencing factor of health literacy among older adults (26). Variations in study samples might explain this discrepancy; our study included adults aged 18 years and above, while Chiu et al. included those above 65 years (21,26). Besides, we found no significant difference in OSA-related health literacy based on the duration of diagnosed OSA (<4 vs. ≥4 years). When comparing with other studies, we did not find research exploring the association between the duration of diagnosis and OSA-related health literacy, except for a study by Yu et al., which reported that OSA participants with a longer duration of the disease demonstrated higher levels of self-management in a study population where more than 60% were aged 31–50 years (27). This finding is not directly comparable to our study population, where over 70% were aged above 50 years.
Second, most participants reported they needed to improve their health and related health habits. This reflects a strong demand for knowledge transfer for OSA and related diseases to improve health literacy, and health behaviour change programs. Studies show that OSA participants who received motivational enhancement education were more likely to adhere better to CPAP treatment, with greater improvements in treatment self-efficacy and daytime sleepiness (28,29).
Third, 71.4% believed e-health information could remind them to improve their health-related habits, and 73% were willing to share the received health messages with family or friends. Hong Kong has extensive smartphone penetration (97.1% in 2022) (30), and strong evidence supports the value of mobile text messaging in managing chronic illness (31). However, in our current services, existing OSA education programs are conducted via face-to-face sessions focusing either on CPAP adherence or lifestyle modification, but not both. The World Health Organization recommends empowering patients to engage and collaborate in self-management to build capacity in managing chronic illness. Thus, this study provides a strong foundation for smartphone-based messaging interventions to benefit a greater population.
Strengths and limitations
The strength of this study lies in understanding preferences for the timing and frequency of receiving instant messages. This will help us determine an appropriate schedule for sending messages to OSA participants and aid in designing, developing, and implementing a smartphone-based self-management support program. Participants’ willingness to share health information with friends and family suggests that mobile instant messaging could be a cost-effective way to promote OSA-related health information. Additionally, qualitative feedback indicated that participants appreciated short, informative videos, which improved health literacy and motivated lifestyle changes by highlighting the link between OSA and other diseases. However, a review on the effect of patient education videos on modifying health behaviours noted a lack of robust studies reporting reliable or sustained effects (32). Thus, our findings can contribute to the co-design of a patient-centred, robust, theoretically underpinned smartphone-based self-management program that targets improvements in patients’ overall health, sleep apnoea, and related conditions.
Our study has several limitations that should be acknowledged. First, as a cross-sectional study with no longitudinal follow-up, causal relationships could not be established. Second, potential selection bias could not be eliminated due to the non-probability, convenient sampling method and the small sample obtained from a single hospital. Additionally, this study was conducted at the beginning of the coronavirus disease (COVID) pandemic; we are forced to stop the survey due to the infection control policies. Third, the lack of significant differences by age or disease duration may reflect limited statistical power due to the small sample size. This sampling method, combined with the small sample size, limited both the reliability and generalizability of the findings. Future studies should recruit a more diverse, representative, and larger sample from hospitals in different regions to minimize such biases. Stratified sampling techniques could also be employed to ensure representation across different demographics, such as age, gender, socioeconomic status, and geographic location. Fourth, the study was conducted in urban Hong Kong, where participants generally exhibit high technology adoption rates and better health literacy. As a result, the findings may not be generalizable to low-income countries or rural areas, where differences in health literacy and social environments could affect the applicability of the results. Therefore, the results should be cautiously generalized to other age groups, geographic locations, or socioeconomic contexts. Fifth, the cohort was male-dominated, reflecting the natural prevalence of OSA, with male-to-female ratios ranging from 3:1 to 5:1 in the general population (33). However, future studies should aim for more balanced recruitment across genders, as well as different age groups and educational backgrounds, to ensure more comprehensive insights. Finally, this study relied on non-validated, single-item health literacy measures, which may have limited the reliability of the findings. This limitation arose partly due to the lack of a validated OSA-specific questionnaire to assess information preferences. Instead, preferences were measured using outcome-based questions without generating a summative score. While findings from Cordasco et al. suggest that single-item health literacy screeners may be effective for presenting health information to individuals regardless of their health literacy levels (34), future research should consider using validated multi-item tools to improve robustness.
Practical implications
First, the study addresses health literacy gaps, highlighting the need to improve understanding of OSA-related diseases and health-related habits, and emphasizing the importance of tailored health education for better self-management. Second, it provides insights into patients’ perceived needs and information preferences, which can guide the development of personalized, patient-centered, and effective interventions to support health improvement. Third, it suggests a promising smartphone-based, innovative video messaging solution for delivering health information, enhancing treatment adherence, and improving overall outcomes for individuals with OSA.
Conclusions
This study is the first to explore OSA individuals’ health literacy, health-related habits, perceived needs, information preferences, and the acceptability of messaging interventions. Findings highlight low OSA-related health literacy and a strong demand for authoritative health information, and most found that messaging interventions were acceptable for improving health habits and symptoms.
Acknowledgments
The authors thank all the patients who participated in the study. The publication fee is supported by Hong Kong Metropolitan University.
Footnote
Data Sharing Statement: Available at https://mhealth.amegroups.com/article/view/10.21037/mhealth-25-26/dss
Peer Review File: Available at https://mhealth.amegroups.com/article/view/10.21037/mhealth-25-26/prf
Funding: None.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://mhealth.amegroups.com/article/view/10.21037/mhealth-25-26/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. Ethics approval was obtained from the Institutional Review Board of the University of Hong Kong/Hospital Authority Hong Kong West Cluster (No. UW 20-068). This study was conducted in accordance with the Declaration of Helsinki and its subsequent amendments or comparable ethical standards. All participants provided written informed consent.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Benjafield AV, Ayas NT, Eastwood PR, et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med 2019;7:687-98. [Crossref] [PubMed]
- Yeghiazarians Y, Jneid H, Tietjens JR, et al. Obstructive Sleep Apnea and Cardiovascular Disease: A Scientific Statement From the American Heart Association. Circulation 2021;144:e56-67. [Crossref] [PubMed]
- Gottlieb DJ, Punjabi NM. Diagnosis and Management of Obstructive Sleep Apnea: A Review. JAMA 2020;323:1389-400. [Crossref] [PubMed]
- Giampá SQC, Lorenzi-Filho G, Drager LF. Obstructive sleep apnea and metabolic syndrome. Obesity (Silver Spring) 2023;31:900-11. [Crossref] [PubMed]
- Messineo L, Bakker JP, Cronin J, et al. Obstructive sleep apnea and obesity: a review of epidemiology, pathophysiology and the effect of weight-loss treatments. Sleep Med Rev 2024;78:101996. [Crossref] [PubMed]
- Yuan F, Zhang S, Liu X, et al. Correlation between obstructive sleep apnea hypopnea syndrome and hypertension: a systematic review and meta-analysis. Ann Palliat Med 2021;10:12251-61. [Crossref] [PubMed]
- Qie R, Zhang D, Liu L, et al. Obstructive sleep apnea and risk of type 2 diabetes mellitus: A systematic review and dose-response meta-analysis of cohort studies. J Diabetes 2020;12:455-64. [Crossref] [PubMed]
- Zeng X, Ren Y, Wu K, et al. Association Between Smoking Behavior and Obstructive Sleep Apnea: A Systematic Review and Meta-Analysis. Nicotine Tob Res 2023;25:364-71. [Crossref] [PubMed]
- Ko J, Lim JH, Kim DB, et al. Association between alcohol use disorder and risk of obstructive sleep apnea. J Sleep Res 2024;33:e14128. [Crossref] [PubMed]
- Hudgel DW, Patel SR, Ahasic AM, et al. The Role of Weight Management in the Treatment of Adult Obstructive Sleep Apnea. An Official American Thoracic Society Clinical Practice Guideline. Am J Respir Crit Care Med 2018;198:e70-87. [Crossref] [PubMed]
- de Zambotti M, Cellini N, Goldstone A, et al. Wearable Sleep Technology in Clinical and Research Settings. Med Sci Sports Exerc 2019;51:1538-57. [Crossref] [PubMed]
- Ghelani DP, Moran LJ, Johnson C, et al. Mobile Apps for Weight Management: A Review of the Latest Evidence to Inform Practice. Front Endocrinol (Lausanne) 2020;11:412. [Crossref] [PubMed]
- Lou BX, Greenberg H, Korotun M. Advances in Treatment of Sleep-Disordered Breathing. Am J Ther 2021;28:e196-203. [Crossref] [PubMed]
- Pépin JL, Bailly S, Tamisier R. Big Data in sleep apnoea: Opportunities and challenges. Respirology 2020;25:486-94. [Crossref] [PubMed]
- Bazoukis G, Bollepalli SC, Chung CT, et al. Application of artificial intelligence in the diagnosis of sleep apnea. J Clin Sleep Med 2023;19:1337-63. [Crossref] [PubMed]
- Eberle C, Löhnert M, Stichling S. Effectiveness of Disease-Specific mHealth Apps in Patients With Diabetes Mellitus: Scoping Review. JMIR Mhealth Uhealth 2021;9:e23477. [Crossref] [PubMed]
- Marcolino MS, Oliveira JAQ, D'Agostino M, et al. The Impact of mHealth Interventions: Systematic Review of Systematic Reviews. JMIR Mhealth Uhealth 2018;6:e23. [Crossref] [PubMed]
- McCabe C, McCann M, Brady AM. Computer and mobile technology interventions for self-management in chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2017;5:CD011425. [Crossref] [PubMed]
- Shaw G, Whelan ME, Armitage LC, et al. Are COPD self-management mobile applications effective? A systematic review and meta-analysis. NPJ Prim Care Respir Med 2020;30:11. [Crossref] [PubMed]
- Yang F, Wang Y, Yang C, et al. Mobile health applications in self-management of patients with chronic obstructive pulmonary disease: a systematic review and meta-analysis of their efficacy. BMC Pulm Med 2018;18:147. [Crossref] [PubMed]
- Zou P, Huang A, Luo Y, et al. Effects of using WeChat/WhatsApp on physical and psychosocial health outcomes among oncology patients: A systematic review. Health Informatics J 2023;29:14604582231164697. [Crossref] [PubMed]
- Dunn J, Coravos A, Fanarjian M, et al. Remote digital health technologies for improving the care of people with respiratory disorders. Lancet Digit Health 2024;6:e291-8. [Crossref] [PubMed]
- Morse JM. Qualitative research methods for health professionals. SAGE Publications; 1995.
- van der Gaag M, Heijmans M, Spoiala C, et al. The importance of health literacy for self-management: A scoping review of reviews. Chronic Illn 2022;18:234-54. [Crossref] [PubMed]
- Dinh TTH, Bonner A. Exploring the relationships between health literacy, social support, self-efficacy and self-management in adults with multiple chronic diseases. BMC Health Serv Res 2023;23:923. [Crossref] [PubMed]
- Chiu HT, Tsai HW, Kuo KN, et al. Exploring the Influencing Factors of Health Literacy among Older Adults: A Cross-Sectional Survey. Medicina (Kaunas) 2020;56:330. [Crossref] [PubMed]
- Yu H, Gao Y, Tong T, et al. Self-management behavior, associated factors and its relationship with social support and health literacy in patients with obstructive sleep apnea-hypopnea syndrome. BMC Pulm Med 2022;22:352. [Crossref] [PubMed]
- Lai AYK, Fong DYT, Lam JCM, et al. The efficacy of a brief motivational enhancement education program on CPAP adherence in OSA: a randomized controlled trial. Chest 2014;146:600-10. [Crossref] [PubMed]
- Lai A, Fong D, Lam J, et al. Long-term efficacy of an education programme in improving adherence with continuous positive airway pressure treatment for obstructive sleep apnoea. Hong Kong Med J 2017;23:24-7.
- Census and Statistics Department. Thematic Household Survey Report No. 77: Information Technology Usage and Penetration. Hong Kong Special Administrative Region; 2023.
- Hall AK, Cole-Lewis H, Bernhardt JM. Mobile text messaging for health: a systematic review of reviews. Annu Rev Public Health 2015;36:393-415. [Crossref] [PubMed]
- Weidmann AE, Sonnleitner-Heglmeier A, Dartsch DC. Effect of patient education videos on modifying medication-related health behaviours: a systematic review using the behaviour intervention functions. Patient Educ Couns 2023;117:107992. [Crossref] [PubMed]
- Bonsignore MR, Saaresranta T, Riha RL. Sex differences in obstructive sleep apnoea. Eur Respir Rev 2019;28:190030. [Crossref] [PubMed]
- Cordasco KM, Homeier DC, Franco I, et al. Health literacy screening of geriatric monolingual Spanish-speaking patients using single-item literacy screening questions and education. Health Educ J 2012;71:597-605. [Crossref] [PubMed]
Cite this article as: Lai AYK, Choi ACM, Lui MMS, Tsoi HWH, Kwok TTO, Sun Y, Ip MSM. Exploring health literacy, perceived needs, information preferences and acceptability of smartphone-based messaging interventions among individuals with obstructive sleep apnoea in Hong Kong: a mixed-method approach. mHealth 2025;11:44.